Monkeypox has been a developing problem for decades and the current global outbreak was avoidable, but the looming threat was largely ignored, according to a leading expert on the virus.
Dr. Anne Rimoin is a UCLA epidemiology professor and has spent the last two decades in the Democratic Republic of Congo working on monkeypox.
She said it was only when the virus spread beyond rural Africa that it sparked a global response.
“This virus has been spreading in marginalized and vulnerable populations [in Africa] for decades, and we’ve done nothing about it,” Rimoin said. “We have known that monkeypox is a potential problem for decades.”
There are now confirmed cases in Europe, Asia, Australia, Africa, the Middle East and South America. The Centers for Disease Control says there are more than 750 monkeypox cases in the U.S. — across almost every state — but Rimoin said this was certainly an undercount because there was not enough testing available.
Monkeypox is rarely fatal and doesn’t generally lead to hospitalization. It is mostly not spread through the air, and people have been getting it from close physical contact.
So public health experts say the U.S. should have been able to handle the outbreak, and that the missteps right now look a lot like the start of the coronavirus pandemic: not enough tests or vaccines readily available, and an incomplete picture of the spread.
“We have no concept of the scale of the monkeypox outbreak in the U.S.,” biologist Joseph Osmundson at New York University told NPR in June.
In response, in late June the CDC said it would “lean forward with an aggressive public health response to the monkeypox outbreak” and activate its emergency operations center.
And on Monday, the CDC said commercial laboratories had now started testing for monkeypox.
“This will not only increase testing capacity but also make it more convenient for providers and patients to access tests,” CDC director Rochelle Walensky said in a statement.
Rimoin questioned why there wasn’t a more concerted effort to address or prepare for the virus years earlier when monkeypox was spreading in rural Africa.
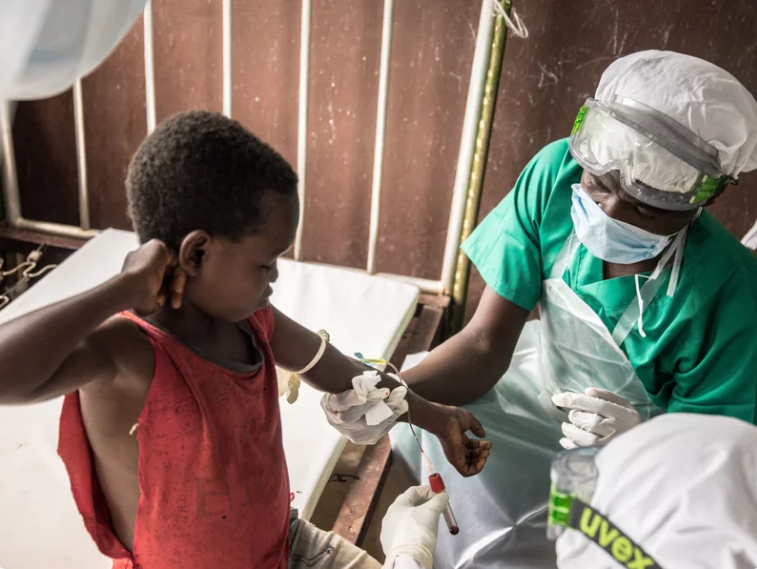
Blood samples are drawn from a boy who didn’t display any sign of monkeypox despite his all family has been contaminated in the Central African Republic in 2018.
She said she had co-authored a paper in 2010 that documented a large increase in monkeypox cases since the eradication of smallpox and the end of the smallpox vaccine, which also protects people from monkeypox.
“If we do want to get in front of emerging infectious diseases, we are going to have to prioritize dealing with emerging global disease threats at the site where they are spreading early on,” Rimoin said. “We are totally interconnected by trade and travel, population growth, population movement, and we cannot make the mistake again of thinking that an infection that’s happening somewhere in a remote area of the world isn’t going to affect us right at home.”
“We will continue to be chasing behind them, and always be paying the price for not doing what’s needed ahead of time.”
For now, Rimoin said it was a matter of trying to contain a virus that was already spreading.
“It’s much easier to stay out of trouble than it is to get out of trouble,” she said.
“The good news is we have vaccines, we have therapeutics, we know a fair amount about this virus. The bad news is now we have to get the logistics together to be able to confront it head on.”
source: https://www.npr.org/2022/07/12/1110897541/monkeypox-outbreak-testing-vaccine-cases
Austin Peter
I am a 23 year old Electronics Engineer. I am also a travel enthusiast and also a webmaster. Please, help my site grow for a better service. Do contact me for financial donations and supports of any kind.
NB: I own this website for I created it from scratch. Although I am currently in partnership with Oset Ventures Group.